Mar 04, 2024

What is Hydronephrosis?
Hydronephrosis is swelling of the kidney that develops due to improper drainage of urine from the kidney to the bladder. This occurs when there is blockage of the outflow or reverse flow (reflux) of the urine. This causes the kidney to swell/enlarge as the urine is unable to pass. Hydronephrosis is due to another disease or disorder and is not considered a primary disease, but a secondary condition.
In the picture below, on the left is a normal kidney/ureter and on the right is hydronephrosis and swelling of the kidney.
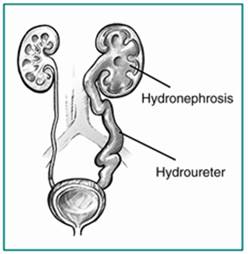
Causes of Hydronephrosis:
Here are some of the most common causes:
- Infection or inflammation of the urethra or urinary tract (UTI)
- Kidney stone
- Congenital disorders
- Pregnancy
- Scarring from previous surgery
- Tumors
- Blood clot
- Enlarged prostate
Symptoms of Hydronephrosis:
- Pain in the abdomen, flank, back and/or bladder
- Fever/chills
- Nausea/vomiting
- Painful urination
- Incomplete voiding or bladder emptying
Treatment for Hydronephrosis:
Treatment is typically focused on treating the underlying condition by removing the urine buildup, relieving pressure, or clearing the infection. If caused by infection, this would be treated with antibiotics. Some kidney stones can be passed without surgery; however, some may require removal or break-up of the stone for removal/passage. A nephrostomy tube may be used to drain the urine from the kidney, or a catheter may be used to drain the urine from the bladder. The most important thing in treatment of hydronephrosis is to get it addressed as soon as it is known to prevent permanent damage to the kidneys.
Coding of Hydronephrosis:
Hydronephrosis
-with
–obstruction (by) (of)
—ureteral NEC N13.1
—–with infection N13.6
—-calculus N13.2
—–with infection N13.6
Etc.
When reviewing the medical record, look for potential causes of hydronephrosis such as stone and infection and report based on the ICD-10-CM Alphabetic Index.
Authored by Kim Boy, RHIT, CDIP, CCS, CCS-P
References
ICD-10-CM Index
ICD-10-CM/PCS Coding Clinic, Second Quarter 2018: Page 21
ICD-10-CM/PCS Coding Clinic, Fourth Quarter 2016: Page 43
https://www.youtube.com/watch?v=sDfL689VPPc
www.kidney.org/atoz/content/hydronephrosis
https://www.healthline.com/health/unilateral-hydronephrosis
https://commons.wikimedia.org/wiki/Main_Page
In need of coding support? We offer both inpatient coding support and outpatient coding support services. Partner with us to replace underperforming coding vendors, get coding backlogs caught up, staff for a FMLA/vacation gap, special projects, to assist in Single Path Coding, or for Total Outsource Coding Support.
The information contained in this coding advice is valid at the time of posting. Viewers are encouraged to research subsequent official guidance in the areas associated with the topic as they can change rapidly.
Subscribe to our Newsletter
Recent Blogs
Related blogs from Industry News , Medical Coding Tips
Coding for treatment of cerebral aneurysms ma...
With the implementation of ICD-10-CM came mor...
It is difficult for coders to know when to re...
Health Information Associates (HIA), known fo...
Subscribe
to our Newsletter
Weekly medical coding tips and coding education delivered directly to your inbox.





Leave a Comment