Sep 25, 2018
What the Index Revels:
When the coder indexes stenosis, carotid the index states “See occlusion carotid.” The coder can see that “with” is linking the cerebral infarction with carotid stenosis in the index:
Occlusion:

When the coder indexes infarction, cerebral, there is the term “due to” listed.This means there must be a link by the physician documented. “Due to” is not assumed to exist without physician documentation.
But there is a “see also” note right next to cerebral (cerebral (see also Occlusion, artery cerebral or precerebral, with infarction) I63.9-). If the coder follows that, they will end up with the combination code.
cerebral (see also Occlusion, artery cerebral or precerebral, with infarction) I63.9-
aborted I63.9
cortical I63.9
due to
cerebral venous thrombosis, nonpyogenic I63.6
embolism
cerebral arteries I63.4-
precerebral arteries I63.1-
occlusion NEC
cerebral arteries I63.5-
precerebral arteries I63.2-
stenosis NEC
cerebral arteries I63.5-
precerebral arteries I63.2-
thrombosis
cerebral artery I63.3-
precerebral artery I63.0-
The tabular has this note:
I63 Cerebral infarction
Includes: occlusion and stenosis of cerebral and precerebral arteries, resulting in cerebral infarction
This note is including both occlusion AND stenosis causing cerebral infarction.
Also in the AHA handbook is an example number 28.5 in which a cerebral infarction is linked “with carotid stenosis” and the one combination code, I63.231 is assigned.
What should the coder do?
In reviewing the case from 3Q2018 Coding Clinic page 5, the MI is not coded as associated with a totally occluded coronary artery because the MI is in a different artery. The MI is coded separately from the total occlusion and is not assumed to be related.
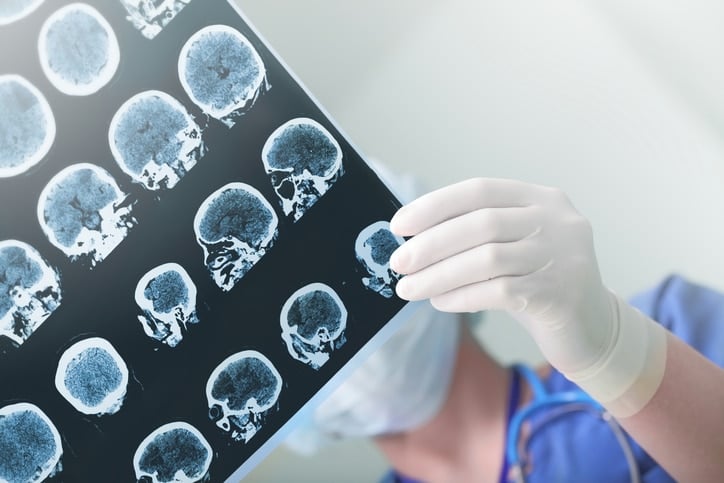
Similarly in a case of cerebral infarction with carotid stenosis, the coder should look at CT scans or MRIs to find the location of the cerebral infarction. If the origination is from the carotid stenosis, and it is documented as such, then the combination code would be assigned. However, if the coder sees that the cerebral infarction is in a different artery than the carotid stenosis, or due to another cause, the cerebral infarction would be coded separately with an additional code for the carotid stenosis. The combination code would NOT be assigned. (i.e. I66.01 and I65.21). Cerebral infarctions can be due to other causes such as a thrombus or embolus that are not related to carotid stenosis. Many patients have minimal carotid stenosis but have cerebral infarctions due to other causes.
When it is unclear, and if the facility allows, best practice would be to query the physician to see if the cerebral infarction is related or unrelated to the carotid stenosis. In the interim, if the record is unclear of a relationship between the cerebral infarction and the carotid stenosis, and the facility does not allow query in these cases, it may be best to assign separate codes for the carotid stenosis and cerebral infarction. This is because the code description itself states “Due to” within it. (i.e. Cerebral infarction due to unspecified occlusion or stenosis of unspecified precerebral arteries). HIA is seeking official guidance on this situation.
References
Coding Clinic 3rd Quarter 2018
ICD-10-CM Official Guidelines for Coding and Reporting
In need of coding support? We offer both inpatient coding support and outpatient coding support services. Partner with us to replace underperforming coding vendors, get coding backlogs caught up, staff for a FMLA/vacation gap, special projects, to assist in Single Path Coding, or for Total Outsource Coding Support.
The information contained in this post is valid at the time of posting. Viewers are encouraged to research subsequent official guidance in the areas associated with the topic as they can change rapidly.
Subscribe to our Newsletter
Recent Blogs
Related blogs from Medical Coding Tips
Debridement is the medical removal of dead, d...
Coding for treatment of cerebral aneurysms ma...
With the implementation of ICD-10-CM came mor...
It is difficult for coders to know when to re...
Subscribe
to our Newsletter
Weekly medical coding tips and coding education delivered directly to your inbox.






Leave a Comment